Can Stress Cause Physical Pain?
This week is Mental Health Awareness Week — and I wanted to use it as an opportunity to talk about something I see in clinic every single day, but that rarely gets spoken about openly: the very real, very physical impact that stress has on your body.
The Connection Most People Miss
When you're stressed, you feel it physically. Tight shoulders. A clenched jaw. That churning feeling in your stomach. Most people reach for a painkiller or book a massage — and while that might take the edge off, it rarely solves the problem. Because the problem isn't the symptom. The problem is what's driving it.
It's worth knowing that around 80% of musculoskeletal pain — back pain, neck pain, shoulder pain — is classified as idiopathic. That means no identifiable structural cause. Which sounds alarming, but is actually good news, because it points us toward something we can genuinely work on.
Your Nervous System Is the Starting Point
To understand how stress causes physical pain, you need to understand the autonomic nervous system — the part of your nervous system that runs in the background, regulating everything from your heart rate to your digestion.
It has two modes:
Sympathetic — fight, flight or freeze. This is your emergency response system. It floods your body with adrenaline and cortisol, raises your heart rate, tightens your muscles, and redirects blood away from digestion and toward your limbs so you can run or fight.
Parasympathetic — rest and digest. This is your recovery mode. Heart rate slows, digestion resumes, muscles relax, tissue repair happens.
The problem is that modern life keeps us chronically stuck in sympathetic dominance. Deadlines, screens, financial pressure, poor sleep, difficult relationships — your nervous system doesn't distinguish between a lion chasing you and a difficult email. As Robert Sapolsky explores in his book Why Zebras Don't Get Ulcers, the stress response that kept our ancestors alive is the same one being triggered dozens of times a day by the demands of modern life.
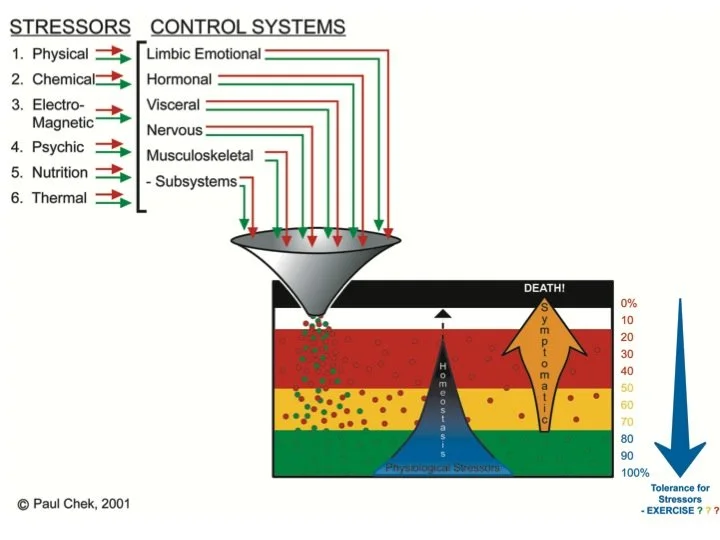
The Accumulation Problem — Allostatic Load
Here's something that doesn't get talked about enough. Small stresses on their own are manageable. But they accumulate.
Poor sleep. Poor diet. Not enough water. Not enough movement. A difficult relationship. Financial worry. Each one alone might be tolerable — but stacked on top of each other, they create what medicine calls allostatic load: the cumulative burden of chronic stress on the body and mind.
Paul Chek has written and spoken about this for years, referring to it as physiological load. At Evolve Osteopathy, understanding a patient's total load — not just their physical symptoms — is central to how we assess and support people. The more stress your body is carrying, the more pain you will experience. That's not a theory, it's physiology.
Image taken from Paul Chek’s Book “How to Eat Move and Be Healthy”
How Stress Creates Physical Pain — System by System
Muscle Tension
When you're stressed, your body increases muscle tone as a protective response. The most common holding areas are the neck, shoulders and jaw. Over time this leads to restricted movement, joint compression and pain — and crucially, bracing patterns that become habitual. Even when the original stressor has gone, the body continues to brace in anticipation of it. Massage and manual therapy can bring relief, but if the underlying stress isn't addressed, the tension will keep coming back.
Breathing and Chest Pain
Stress changes your breathing pattern. Calm, diaphragmatic breathing — slow, deep, driven by the diaphragm — shifts to faster, shallower upper chest breathing. This overworks the accessory respiratory muscles: the scalenes, sternocleidomastoid, and upper trapezius. The diaphragm — innervated at C3, C4 and C5 in the neck — becomes underused, contributing to neck tension and further reinforcing the stress response.
Anxiety can also directly mimic cardiac symptoms — chest tightness, palpitations, shortness of breath. This creates a vicious cycle: the physical sensations cause more anxiety, which drives more adrenaline and cortisol, which intensifies the symptoms. If you're experiencing chest pain, it's always important to get checked out medically to rule out an underlying heart or lung condition — but in many cases, stress is the primary driver.
Headaches
Sustained muscle tension reduces blood supply to the muscles of the upper neck and base of the skull. This ischaemia — combined with jaw clenching and altered neck mechanics — is a primary driver of both tension-type headaches and cervicogenic headaches. Stress also lowers your pain threshold, meaning the same stimulus hurts more when you're under pressure. This is central to understanding conditions like fibromyalgia and chronic fatigue syndrome, where long-term stress has fundamentally altered the nervous system's sensitivity to pain.
Gut Health
The gut and brain are in constant two-way communication via the vagus nerve — the tenth cranial nerve, running from the brainstem deep into the abdomen and powered primarily by the parasympathetic nervous system. When we're stressed, this communication is disrupted. IBS flare-ups, bloating, and digestive discomfort are frequently stress-driven — and this is increasingly well understood clinically.
What's less well known is that the gut contains its own independent nervous system — the enteric nervous system, sometimes called the second brain. The vast majority of the body's serotonin — the neurotransmitter most associated with mood and wellbeing — is produced in the gut. When gut health is compromised, serotonin production can be affected, which has direct implications for anxiety, depression and pain sensitivity. Gut inflammation doesn't just affect digestion. It affects how you feel, how you cope, and how much pain you experience.
What This Means for Your Treatment
If you've had treatment for a physical problem and it keeps coming back, stress may be the missing piece. At Evolve Osteopathy, we don't just assess where it hurts — we assess the whole picture. That includes your sleep, your stress levels, your breathing, your nutrition, and your lifestyle — because all of these things feed into how your body feels and how well it recovers.
This is the foundation of the three-phase approach we use: moving from Pain Relief, through Corrective Care, and into long-term Wellness — addressing not just the symptom but the conditions that created it.
This Mental Health Awareness Week
Your mental health and your physical health are not separate. They never were. If your body is sending you signals — persistent pain, tension that won't shift, headaches that keep coming back — it's worth asking what your nervous system might be trying to tell you.
If you'd like to find out more or book an initial consultation, visit evolveosteopathy.co.uk